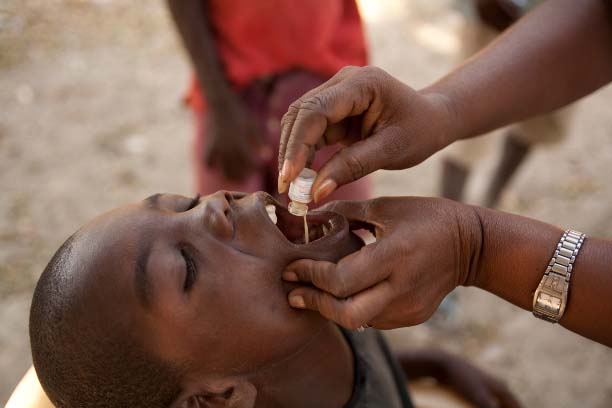
The world’s worst cholera outbreak highlights need for long-term solutions
|

In 2015, civil war broke out in Yemen between the government and the rebel movement, triggering a humanitarian crisis that has resulted in more than 70 per cent of the population needing immediate aid and assistance. Yemen is one of the poorest countries in the Arab peninsula, and constant bombings have devastated infrastructure, including roads and hospitals.
One of the most devastating consequences of this war and instability has been the worst cholera outbreak ever recorded. Cholera is an acute diarrhoeal disease that thrives in disadvantaged and unstable environments; it can kill within hours if left untreated. Malnutrition and poor sanitation have made the country vulnerable to cholera, and more than 800,000 civilians have already been affected. The World Health Organization (WHO) expects this number to rise to a million by the end of the year.
Many local medical professionals have fled the country, and those who have remained work around the clock and without pay. Other challenges have also arisen: Oral cholera vaccines, which are the internationally accepted method of controlling a cholera epidemic, were scheduled to be deployed in June 2017, but the difficulties of delivering a mass immunization campaign in conflict-ridden areas has prevented distribution.
The precarious security situation has also prevented a team from icddr,b from being deployed to the country. In October, the Kuwaiti Women Philanthropic Team sponsored a visit of Yemeni doctors and nurses for a training course in Dhaka, Bangladesh at icddr,b. The weeklong hands-on training on cholera and malnutrition case management focused on outbreak control and prevention, surveillance methods, case management, and awareness of waste management and sanitation systems. The participants also observed management of cholera and other watery diarrhea and learned about dehydration assessment, severe acute malnutrition, food preparation, child feeding practices, and community-based management of illnesses.
Yemen is not the only country currently facing an emergency threat from diarrheal disease. icddr,b scientists are currently working with our government and other organizations to prevent a cholera outbreak in Cox’s Bazar in southern Bangladesh by distributing cholera vaccines to Rohingya refugees who have been arriving from Myanmar since August. The teams will administer over 900,000 doses of the vaccine, making this the second largest oral vaccination campaign in the world after Haiti in 2016.
The threat of cholera is an opportunity to bring attention to the danger of diarrhea and the current tools we have to address epidemics. In addition to cholera vaccine for prevention, one of the most effective mechanisms for treating diarrhea is oral rehydration solution (or ORS), an innovation developed by icddr,b in the 1970s that has saved more than 50 million lives.
However, short-term management of epidemics is not enough. For the long term, a holistic approach is needed, which includes access to safe drinking water, improved sanitation, promotion of proper hygiene, and overall health awareness about how infections spread. Globally, 2.1 billion people lack access to safe water and more than double that number are without safe sanitation. We also need greater collective advocacy on the rotavirus vaccine. Nearly 40 per cent of countries in Africa have yet to introduce the vaccines despite more than half of all global rotavirus deaths occurring in Africa. Asia, too, has a very high prevalence for rotavirus, but only 20 per cent of its countries have introduced it to the population.
In emergency situations, vaccination campaigns and training on cholera management and treatment can provide vital support, but only long-term adoption of these interventions will ensure disease outbreaks like cholera become a thing of the past.
Photo credit: PATH/Doune Porter.