
Ten Years On: How Have Rotavirus Vaccines Impacted Diarrhea Cases?
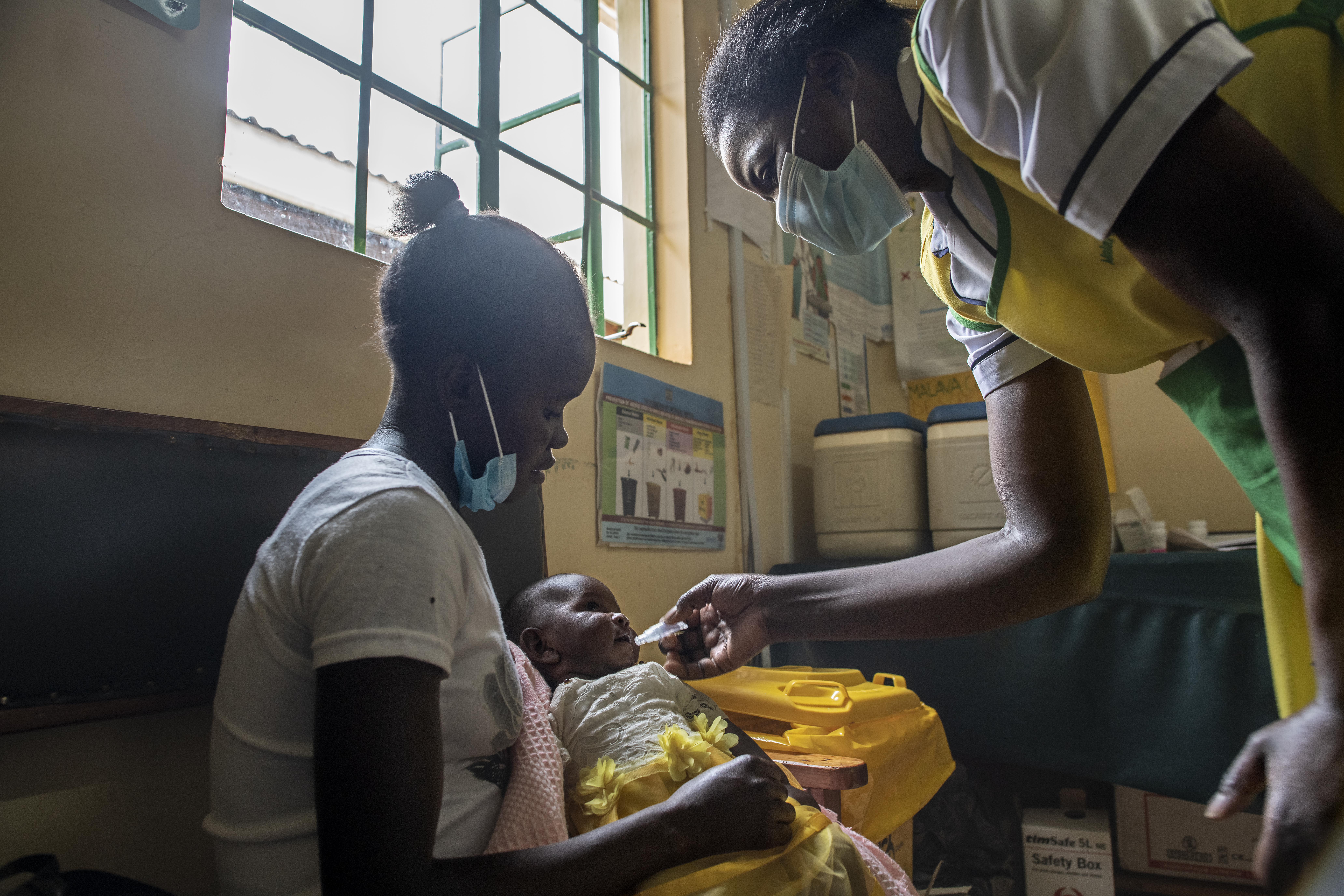
A nurse administers a rotavirus vaccine in Kakamega County, Kenya. Photo: PATH/Anthony Karumba.
Nearly all African countries have introduced rotavirus vaccines or plan to do so within the next couple of years. The vaccines are safe, effective, and reaching more children than ever before. But rotavirus still tops the list of pathogens responsible for deadly diarrhea in sub-Saharan Africa. It kills 160,000 African children every year, and hospitalizes many more.
Vaccines have made powerful progress, but oral vaccines like rotavirus do not perform as well in low-resource countries. Rotavirus is also not nearly the only cause of childhood diarrhea. Shigella, norovirus, E. coli, and cryptosporidium are also prevalent. New vaccines and treatments against these pathogens are under development, as are improved rotavirus vaccines. In the interim, countries and communities must prioritize access to tried-and true interventions that block diarrhea’s deadly path: water, sanitation, and hygiene (WASH), Oral Rehydration Solution (ORS)/zinc, and improved nutrition.
As scientific experts noted in a recent supplement to the Journal of Clinical Infectious Diseases, “We see a convergence of factors, including lack of real progress with access to ORS, substantial improvements in WASH interventions, access to appropriate medical care, or improved nutrition that make African children particularly vulnerable to severe diarrheal disease and associated poor outcomes.” The journal supplement collated data from the groundbreaking VIDA study, which evaluated the impact of rotavirus vaccines in three African countries.
VIDA investigates life-saving solutions
The VIDA study looked closely at communities to elucidate the clinical and epidemiological factors of moderate to severe diarrhea. In three countries (The Gambia, Kenya, and Mali), researchers not only evaluated incidence and pathogens, but also aimed to understand the social and demographic characteristics that heighten children’s risk of infection.
Gambia introduced rotavirus vaccines in 2013, and introductions in Kenya and Mali followed in 2014. The clinical sites participating in the VIDA study had previously reported data to the seminal GEMS study that analyzed diarrhea-causing pathogens from 2007-2011 in sub-Saharan African and Southeast Asia. VIDA represents the first comprehensive review of diarrhea-causing pathogens since those milestones.
“Using the same three sites in sub-Saharan Africa, we have generated data from the region experiencing the highest burden mortality from diarrheal diseases,” explained Dr. Dilruba Nasrin, an associate professor at the University of Maryland School of Medicine Center for Vaccine Development and a co-author on the VIDA study. “By using comparable methodology to elucidate incidence, etiology, and adverse consequences, we can understand the most severe diarrheal episodes and prioritize prevention.”
Overall, VIDA’s results reveal a decline in diarrhea mortality over the past decade. Specific data are forthcoming in a future journal publication. Researchers attributed these gains to changes in social, environmental, and economic conditions, as well as introduction and high coverage of rotavirus vaccines.
But too many children still face the risk of infection by the dangerous pathogens under VIDA’s microscope. No child should die of diarrhea, and evidence of progress alongside persistent obstacles is crucial to spur greater investment. Data unveiled through the VIDA study, the experts conclude, “provides a target and motivation for national health programs to develop focused goals for improvement.” As always, an integrated investment in prevention and treatment, tailored to community-level needs, is the best way to protect children from these everyday infectious threats.


