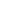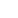Hospitals without water, toilets, or soap make the sick even more vulnerable to infection
|
Medical staff prepping for surgery with limited resources in Kilembe, Uganda. Photo: PATH/Tom de Blasis.
Think back to the last time you visited a doctor’s office or a hospital. Was clean drinking water available? Were there clean, running toilets in the bathrooms? How about sinks in the patient consultation rooms?
In the US, we often overlook how important and central basic infrastructure like safe, running water, working toilets, and accessible sinks and soap in health facilities are to a quality patient experience. We expect health facilities to have these basic items. Try to imagine that same patient visit if there was only a single toilet for an entire hospital that was never cleaned, or having to walk a half mile for safe water, or having doctors and nurses reuse gloves for each patient and/or never wash their hands due to the lack of handwashing sinks and soap.
On Monday, November 5, 2018, a water main near Chapel Hill, North Carolina burst, leaving the city’s households, schools, businesses, and health centers without access to safely treated water. As a result of the break, nearby schools closed and the University of North Carolina (UNC) Hospitals began rerouting trauma patients, cancelling elective surgeries, distributing bottled water to patients and staff, and setting up portable handwashing stations throughout the hospital.
The timing of this event could not have been more striking in light of a key theme from a global water, sanitation, and hygiene conference held a few miles down the road from the break. Just a week before, global water and sanitation experts gathered at the University of North Carolina’s annual Water and Health Conference to present leading research on water, sanitation, and hygiene (WASH) advances across the globe. One of the key themes this year was improving WASH services in health care facilities.
A recent major study by the World Health Organization (WHO) and UNC concluded that only half of all health facilities in low- and middle-income countries have piped water, a third lack adequate toilets, and nearly 40% do not have soap for handwashing. Furthermore, just 2% of these health care facilities can provide a complete service package of appropriate water, sanitation, hygiene, and waste management services. Without clean and safe water, sanitation, and hygiene, patients and providers are at a much higher risk for hospital-acquired infections—3 to 20%—than patients and providers in high-income countries. Without these basic WASH services, quality health care cannot be delivered.
Unlike repairing a broken water main in the US, the challenges for installing and/or improving necessary, basic WASH infrastructure in low- and middle-income health care facilities are much more complex and will require low-cost, innovative solutions. At the Water and Health Conference, a variety of international organizations, the WHO/United Nations Children’s Fund, and national and subnational governments presented on how they are working to address these gaps. Approaches range from high-level political advocacy, and capacity building programs to facility- and health care staff-based service delivery improvements. PATH is contributing to this sector by supporting the introduction and evaluation of innovative WASH technologies in health care facilities.
On your next visit to a doctor’s office or a hospital, take a moment to look around and see how easy it is to access safe drinking water, toilets, and sinks and soap. PATH and many other partners are working to make this reality the norm across the globe.